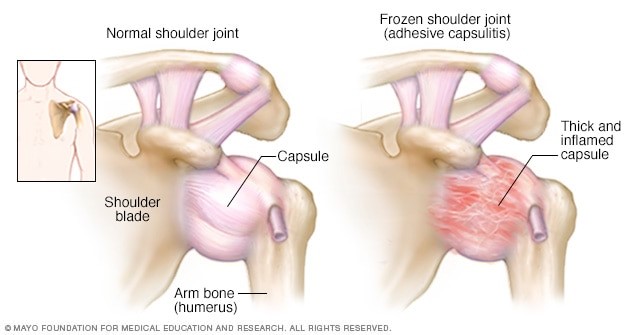
Frozen Shoulder: What it is and what to do about it
Frozen shoulder, also known as adhesive capsulitis, is characterized by pain and global loss of shoulder joint range of motion. The strong connective tissues surrounding he shoulder joint (known as the joint capsule) become thickened, stiff and inflamed. This process leads to progressive joint stiffness and significant decrease in range of motion which can affect one’s ability to perform activities of daily living such as dressing or grooming.
There are two types of frozen shoulder (FS), primary and secondary. Primary is generally idiopathic (occurs with no known cause). Secondary generally arising from a known cause, predisposing factor or traumatic event. Common causes associated with secondary FS include diabetes, hypothyroidism and metabolic syndrome. Frozen shoulder is more prevalent in woman, who make up 70% of individuals who present with FS. Diagnosis of frozen shoulder is more prevalent in patients 35-65 years old, with an occurrence rate of 2-5% of the general population.
Patient who present to the clinic with FS typically report insidious onset with progressive pain and decreased function. These patients typically report difficulty reaching overhead, reaching behind their body and/or difficulty lifting heavy objects. FS literature states that this disorder progresses throughout three overlapping phases, each with their own clinical characteristics:
- Acute/freezing/painful phase: this phase is characterized by gradual onset of pain at rest, pain at night that causes difficulty sleeping. Can last 2-9 months
- Adhesive/frozen/stiffening phase: Pain slowly decreases, however there is progressive loss of shoulder motion. Can occur 4 months- 12 months
- Resolution/thawing phase: Spontaneous, progressive improvement in shoulder motion. Some studies suggest this phase can last up to 3 years after the onset of symptoms.
If a patient experiences pain and loss of function, they should be evaluated by a physical therapist (PT) who will take them throughout a full orthopedic assessment to determine if the patient is suffering from FS. It is important that patients understand although they may never regain full motion of the affected shoulder, the condition will spontaneously resolve and the stiffness will decrease over time. What is done in the clinic will depend on a patient’s presentation including which phase they are in.
- Initial phase: painful, freezing: pain relief is the major goal during this phase. Gentle manual therapy, soft tissue work, and modalities (heat, ice) are utilized to decrease a patient’s pain. Activities that increase symptoms shoulder be avoided.
- Second phase: decreased motion: gentle, progressive stretching exercises are performed by the PT and patient. Care must be taken to avoid aggravating the shoulder.
- Third phase: resolution: gentle strengthening exercises can be introduced into the plan of care once pain has subsided. Patients are told to hold stretches for longer durations and frequencies.
Developing frozen shoulder can be scary and seem like a daunting task to undertake alone. However, research has shown physical therapy significantly decreases pain and increased function. For more information, please contact your local orthopedic physical therapist for an assessment to see if you have developed FS and begin the journey back to performing your favorite activities with less pain. Physical Therapists improve the way you move!
Ryan Hastie, PT, DPT, CSCS
Doctor of Physical Therapy
Certified Strength and Conditioning Specialist
Titleist Performance Institute Medical 2 Certified